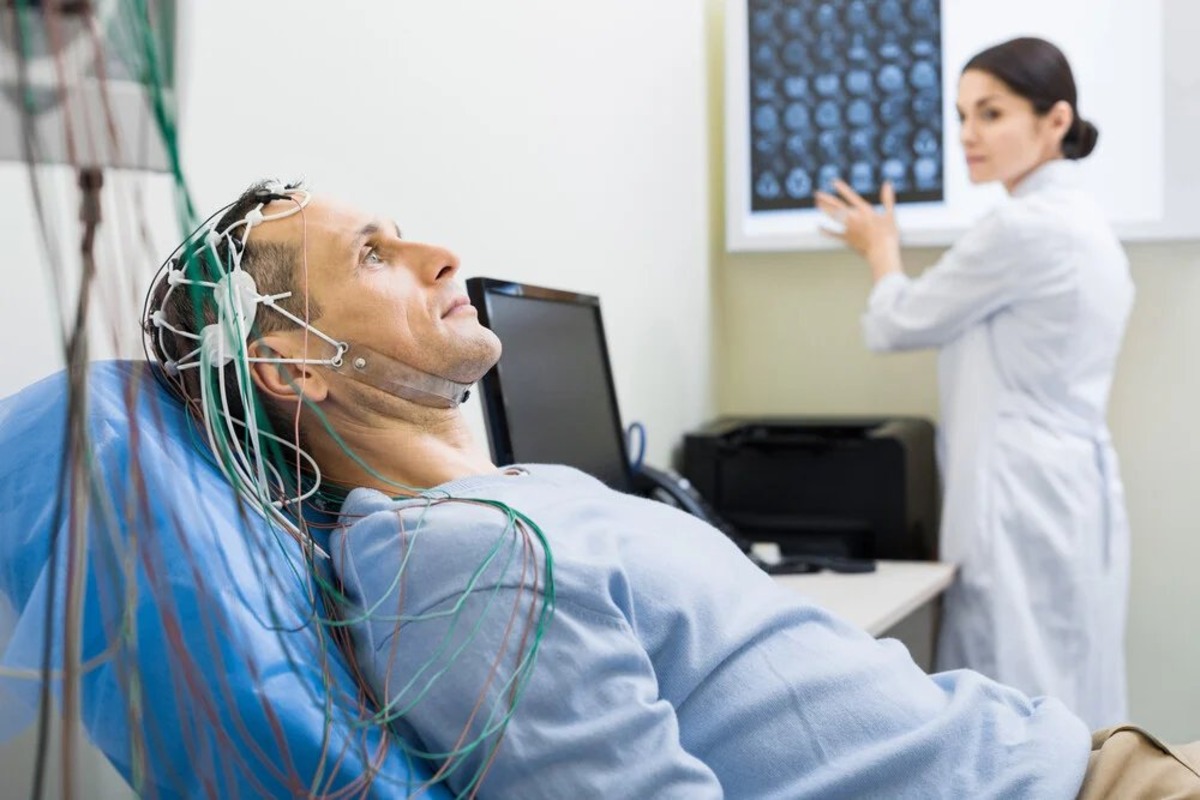
Medical School
Attending medical school is the first step on the path to becoming a neurologist. This rigorous and comprehensive educational program equips aspiring neurologists with the necessary knowledge and skills needed to diagnose and treat disorders of the nervous system.
To gain admission to medical school, aspiring neurologists must first complete a bachelor’s degree in a pre-medical or related field. While there is no specific undergraduate major required, coursework in biology, chemistry, physics, and mathematics is highly recommended. Additionally, applicants must achieve a competitive score on the Medical College Admission Test (MCAT).
Once accepted into medical school, aspiring neurologists embark on a four-year journey of intensive study and clinical training. The first two years typically consist of classroom-based instruction, focusing on foundational sciences such as anatomy, physiology, pharmacology, and pathology. Students also gain exposure to clinical skills through simulations and laboratory sessions.
The last two years of medical school are spent in clinical rotations, where students rotate through various medical specialties, including neurology. During these rotations, students have the opportunity to work directly with patients under the guidance of experienced physicians. This hands-on experience allows students to develop essential clinical skills and gain a deeper understanding of neurologic disorders.
Throughout their medical school education, aspiring neurologists are also encouraged to engage in research and scholarly activities. This may involve conducting neurology-related research studies, presenting findings at conferences, or publishing articles in medical journals. Participation in these scholarly activities demonstrates a commitment to advancing the field of neurology.
Upon successful completion of medical school, graduates are awarded the Doctor of Medicine (M.D.) or Doctor of Osteopathic Medicine (D.O.) degree. However, their journey to becoming a neurologist is far from over.
Residency Program
After completing medical school, aspiring neurologists must embark on a residency program to gain specialized training in neurology. A neurology residency typically lasts for four years and provides an in-depth, hands-on experience in diagnosing, treating, and managing neurological disorders.
During the residency program, residents work closely with experienced neurologists and faculty members in various clinical settings. They rotate through different neurology subspecialties, including stroke, epilepsy, movement disorders, neuromuscular, and pediatric neurology. This diverse exposure allows residents to acquire comprehensive knowledge and skills across the spectrum of neurology.
In addition to clinical rotations, residents are expected to actively participate in educational activities, such as attending lectures, conferences, and case discussions. They also have opportunities for research and scholarly pursuits, contributing to the advancement of the field through publications and presentations.
Throughout the residency program, residents gain practical experience in conducting neurological examinations, interpreting neuroimaging studies, and formulating treatment plans. They have the chance to work with patients with different neurological conditions, honing their diagnostic and therapeutic skills under the guidance of experienced mentors.
Residents often have the opportunity to work in specialized neurology clinics and hospitals, where they treat patients with specific neurologic disorders. They learn to manage acute neurological emergencies, perform procedures like lumbar punctures, and develop proficiency in interpreting electroencephalograms (EEGs) and other neurophysiological studies.
As the residency progresses, residents gradually shoulder more responsibilities, taking on a leadership role in patient care and decision-making. They collaborate with interdisciplinary healthcare teams, including neurosurgeons, psychiatrists, and rehabilitation specialists, to provide comprehensive and integrated care for patients.
At the end of the residency program, residents are required to pass the board certification examination in neurology to become board-certified neurologists. This examination evaluates their knowledge, clinical skills, and ability to provide quality care to patients with neurological disorders.
Fellowship
Once neurologists complete their residency program, they have the option to pursue further specialized training through a fellowship program. Neurology fellowships offer advanced training in specific subspecialties of neurology and allow neurologists to develop expertise in a particular area of interest.
Neurology fellowships typically range from one to two years, depending on the subspecialty. Some common subspecialties include neurocritical care, movement disorders, epilepsy, neuromuscular disorders, neuroimaging, sleep medicine, and stroke.
During the fellowship, neurologists work under the guidance of experienced faculty members who are experts in their respective subspecialties. They gain exposure to a wide range of complex cases and have the opportunity to develop specialized skills and knowledge in their chosen area.
Fellows participate in clinics, where they evaluate and manage patients with specific neurological conditions. They also have the chance to perform specialized procedures and diagnostic tests relevant to their subspecialty. For example, neurology fellows focusing on epilepsy may perform and interpret video-EEG monitoring, while those in neuroimaging fellowships may become proficient in advanced neuroimaging techniques.
In addition to clinical experiences, fellows are encouraged to engage in research and scholarly activities to contribute to the advancement of knowledge in their subspecialties. This may involve conducting original research studies, collaborating with other researchers, presenting findings at conferences, and publishing articles in medical journals.
The fellowship period also provides opportunities for neurologists to expand their professional network and establish collaborations with other experts in the field. They have the chance to attend conferences, workshops, and symposiums, which offer platforms for knowledge exchange and networking.
By the end of the fellowship, neurologists have gained specialized expertise in their chosen subspecialty. This additional training and experience enhance their clinical skills, research abilities, and overall proficiency in managing patients with complex neurological conditions. As a result, they are better equipped to provide specialized care tailored to the unique needs of patients within their subspecialty.
Licensing and Certification
Obtaining the necessary licensing and certification is a crucial step in the journey to becoming a practicing neurologist. It ensures that neurologists meet the standards and requirements set by regulatory bodies and demonstrates their competence in providing quality care to patients with neurological disorders.
After completing the required education and training, neurologists must obtain a medical license to practice medicine. The specific licensing requirements vary depending on the country or region of practice. Typically, neurologists must pass a licensing examination that assesses their knowledge, skills, and understanding of medical ethics and laws. This examination is usually administered by the medical licensing board or regulatory authority.
In addition to obtaining a medical license, neurologists may also pursue board certification in neurology. Board certification is a voluntary process that validates a neurologist’s expertise and demonstrates their commitment to maintaining high standards of practice. Various specialty boards offer certification in neurology, such as the American Board of Psychiatry and Neurology (ABPN) in the United States.
To become board-certified, neurologists must meet specific eligibility criteria, which typically include completing an accredited residency program and passing a comprehensive board examination. The examination assesses their knowledge, clinical skills, and ability to provide quality care within the field of neurology.
Board certification is not a one-time achievement but requires ongoing maintenance. Neurologists are usually required to participate in continuing medical education (CME) activities to stay updated with the latest advancements and best practices in neurology. They must earn a certain number of CME credits within a specified time period to maintain their board certification.
Furthermore, neurologists may pursue subspecialty certifications if they have completed additional training and meet the requirements set by specialty boards. These subspecialty certifications demonstrate advanced competency in specific areas such as neurocritical care, epilepsy, or vascular neurology.
By obtaining the necessary licensing and certifications, neurologists adhere to professional standards, ensure patient safety, and provide reassurance to their patients that they have met rigorous criteria to practice as qualified and competent neurologists.
Continuing Education Requirements
Continuing education is a vital component of maintaining professional competence and staying up-to-date with advancements in the field of neurology. Neurologists are required to fulfill continuing education requirements to ensure they provide the highest quality of care to their patients.
The specific continuing education requirements vary depending on the country or region of practice, as well as the regulatory body overseeing the medical profession. In the United States, for example, neurologists are required to earn a certain number of Continuing Medical Education (CME) credits every year to maintain their medical license and board certification.
CME activities can take various forms, including attending medical conferences and symposiums, participating in workshops and seminars, engaging in online courses, and reading medical literature. These activities cover a wide range of topics relevant to neurology, such as new research discoveries, emerging treatment modalities, advancements in diagnostic techniques, and updates in neurologic guidelines.
Through continuing education, neurologists have the opportunity to enhance their knowledge and skills, stay abreast of the latest research and evidence-based practices, and adopt new approaches to patient care. It allows them to provide the most current and effective treatments to patients, ensuring optimal outcomes and quality of life.
In addition to providing education, continuing education activities also offer networking opportunities. Neurologists can connect with colleagues, share experiences, and collaborate on research projects or clinical initiatives. This exchange of knowledge and expertise contributes to professional growth and promotes collaboration within the neurology community.
Continuing education requirements also help neurologists identify areas where they may need further training or improvement. By engaging in ongoing learning, they can address any gaps in their knowledge and expand their expertise in specific subspecialties or emerging areas of neurology.
Furthermore, continuing education plays a crucial role in patient safety. It ensures that neurologists are aware of any new safety risks or adverse effects associated with treatments and medications. Neurologists who are well-informed and regularly update their knowledge can provide the most appropriate and evidence-based care, minimizing potential harm to patients.