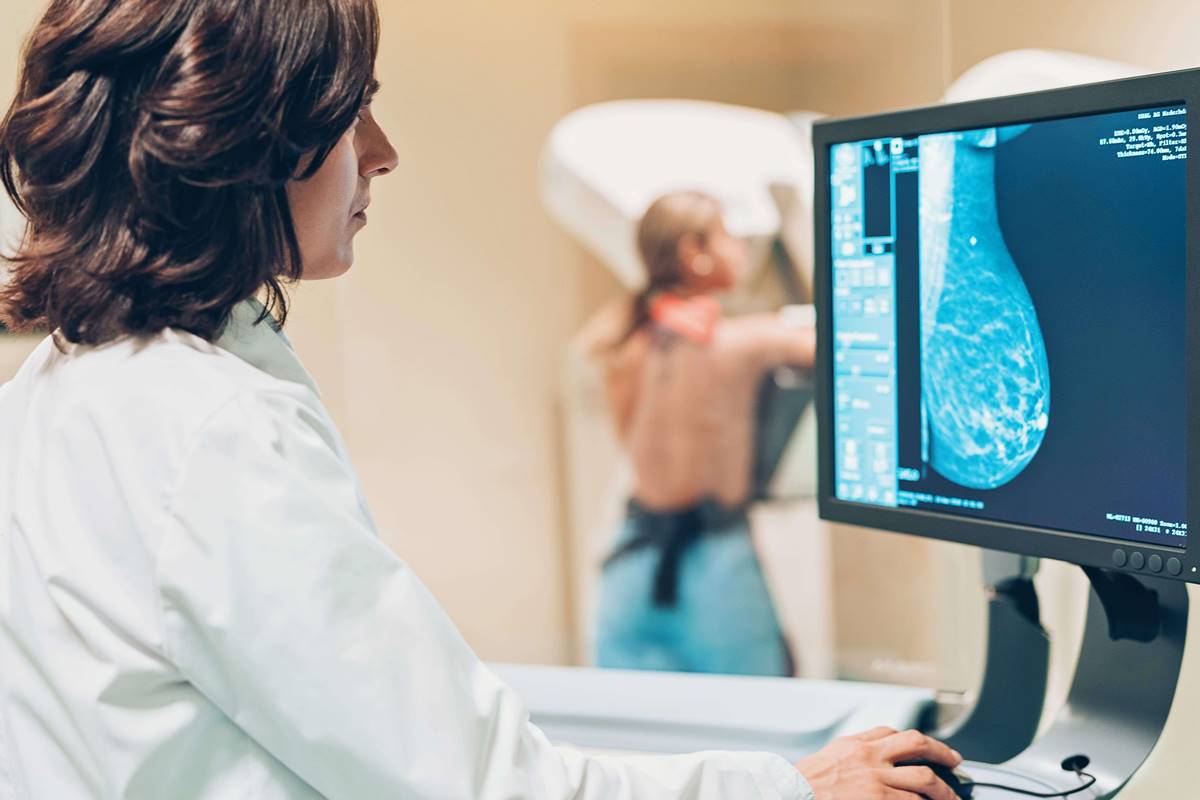
Why Get a Mammogram?
A mammogram is a crucial screening test for the early detection of breast cancer in women. It plays a vital role in identifying any abnormalities or changes in breast tissue that may indicate the presence of cancer cells. While it is true that some women may feel anxious or uncomfortable about undergoing a mammogram, the benefits far outweigh any temporary discomfort. Here are some compelling reasons why getting a mammogram is important:
- Early Detection: Mammograms can detect breast cancer in its earliest stages, often before it can be felt as a lump. Detecting cancer early significantly increases the chances of successful treatment and improves long-term survival rates.
- Early Treatment: Finding breast cancer early through mammography allows for more treatment options and less invasive procedures. Early-stage cancers are often easier to treat successfully, resulting in better outcomes for patients.
- Saving Lives: Regular mammograms have been proven to save lives by reducing breast cancer mortality rates. By detecting cancer in its early stages, treatments can be initiated promptly, leading to improved outcomes.
- Peace of Mind: For many women, undergoing regular mammograms brings peace of mind and reassurance. Knowing that they are taking proactive steps towards maintaining their breast health can alleviate anxiety and provide a sense of control.
- Genetic Risk: Women with a family history of breast cancer or those with certain genetic mutations, such as BRCA1 or BRCA2, may be at higher risk of developing the disease. Mammograms can help detect cancer early in these high-risk individuals, enabling them to take appropriate preventive measures.
Ultimately, a mammogram is a powerful diagnostic tool that helps identify breast cancer at an early stage, allowing for timely treatment and better outcomes. It is essential for women to prioritize their breast health and follow recommended screening guidelines to detect any potential issues as early as possible.
What Is Digital Mammography?
Digital mammography, also known as full-field digital mammography (FFDM), is an advanced imaging technique used to capture and analyze breast images. It involves the use of electronic detectors instead of traditional X-ray films, transforming X-ray images into digital signals for enhanced viewing, interpretation, and storage. This technology has revolutionized breast cancer screening, offering several advantages over conventional film mammography.
With digital mammography, the breast is compressed in the same way as in traditional mammography. However, instead of film, the X-ray images are captured as electronic images and displayed on a computer screen. This digital format allows radiologists to manipulate and enhance the images for improved visualization of breast tissue, leading to more accurate and precise diagnoses.
One of the primary benefits of digital mammography is its ability to produce high-quality images with exceptional clarity. This enables radiologists to detect even the smallest abnormalities or calcifications in the breast tissue, which may indicate early signs of breast cancer. Additionally, digital mammograms can be easily stored, transferred, and accessed electronically, facilitating seamless communication between healthcare providers and reducing the risk of lost or misplaced films.
Another advantage of digital mammography is its lower radiation dose compared to film mammography. The digital technology ensures that the radiation exposure is minimized, while still delivering images of excellent diagnostic quality. This is particularly beneficial for women who may require frequent mammograms or those at higher risk for breast cancer.
In recent years, digital breast tomosynthesis (DBT), also known as 3D mammography, has become increasingly popular. This advanced form of digital mammography captures multiple images of the breast from different angles, creating a three-dimensional reconstruction. DBT provides radiologists with a more detailed view of the breast tissue, reducing the chances of false-positive results and improving the accuracy of cancer detection.
Overall, digital mammography is a significant advancement in breast imaging technology, offering improved image quality, better diagnostic accuracy, reduced radiation exposure, and seamless integration into digital healthcare systems. It has revolutionized breast cancer screening and plays a pivotal role in promoting early detection and improved outcomes for women at risk of breast cancer.
Benefits of Digital Mammography
Digital mammography offers numerous benefits over traditional film mammography, making it a preferred choice for breast cancer screening. Here are some key advantages of digital mammography:
- Improved Image Quality: Digital mammography produces high-resolution images that offer enhanced clarity and detail. This allows radiologists to detect small abnormalities and calcifications more accurately, leading to earlier detection of potential breast cancers.
- Advanced Image Manipulation: The digital format of mammograms allows for easy manipulation of images. Radiologists can adjust the brightness, contrast, and zoom in on specific areas, improving their ability to analyze and interpret breast tissue. This flexibility helps reduce the chances of missed or misinterpreted findings.
- Easier Storage and Retrieval: Digital mammograms can be digitally stored and easily retrieved when needed. This eliminates the need for physical film storage, reduces the risk of lost or damaged films, and enables seamless access to past mammograms for comparison and tracking any changes over time.
- Reduced Radiation Exposure: Digital mammography typically requires a lower radiation dose compared to traditional film mammography. This is beneficial for women who require regular screenings or those at a higher risk for breast cancer, as it minimizes their cumulative radiation exposure while still providing clinically accurate results.
- Improved Workflow Efficiency: The digital format allows for faster image acquisition, processing, and interpretation. Digital mammograms can be viewed instantly on computer screens, eliminating the need for film development and reducing patient wait times. This streamlines the diagnostic process and facilitates prompt communication of results to patients.
- Enhanced Detection of Dense Breast Tissue: Digital mammography is particularly effective in detecting breast abnormalities in women with dense breast tissue. Dense breasts have a higher proportion of glandular and connective tissue, making it more challenging to identify small lesions or cancers on traditional mammograms. Digital mammography offers improved visibility and greater accuracy in detecting abnormalities in dense breast tissue.
The benefits of digital mammography contribute to earlier detection, more accurate diagnoses, and improved outcomes for women undergoing breast cancer screening. By embracing this advanced imaging technology, healthcare providers can provide women with the best possible care and significantly reduce breast cancer mortality rates.
How Does Digital Mammography Work?
Digital mammography is a specialized imaging technique used for breast cancer screening and diagnosis. It involves the use of X-rays to capture detailed images of the breast tissue. Here’s a breakdown of how digital mammography works:
1. Compression: The first step in a mammogram, whether digital or film, is breast compression. The breast is firmly compressed between two plates to spread out the tissue, allowing for better visualization and accurate image capture.
2. X-ray Image Acquisition: Unlike traditional film mammography, digital mammography uses electronic detectors to capture the X-ray image of the breast. These detectors convert X-ray energy into electrical signals, which are then digitized and stored as digital images.
3. Digitization and Image Processing: The digital signals obtained from the detectors are processed and transformed into digital images by specialized computer software. This digitization process allows for further analysis, manipulation, and enhancement of the images for detailed examination.
4. Display on Computer Screen: The digital images are displayed on a computer screen, where radiologists can examine them closely. The images can be zoomed in, adjusted for brightness and contrast, and analyzed meticulously to detect any abnormalities or signs of breast cancer.
5. Storage and Transmission: Digital mammograms can be easily stored and electronically transmitted. They can be stored on computer servers or included in a patient’s electronic health record for future reference and comparison. This digital storage eliminates the need for physical film storage, reducing the risk of loss or damage.
6. Interpretation by Radiologists: Trained radiologists review the digital mammogram images and look for any signs of potential abnormalities. Radiologists rely on their expertise to detect subtle changes, such as masses, microcalcifications, or architectural distortions that may indicate the presence of breast cancer.
Overall, digital mammography improves the process of breast imaging by providing higher image quality, flexibility in image manipulation, and efficient storage and transmission of data. The digitized images allow radiologists to analyze breast tissue in greater detail, enhancing the accuracy of breast cancer screening and diagnosis.
Types of Digital Mammography Systems
There are two primary types of digital mammography systems commonly used in breast cancer screening and diagnosis: Full-Field Digital Mammography (FFDM) and Digital Breast Tomosynthesis (DBT).
1. Full-Field Digital Mammography (FFDM): FFDM is the most widely used digital mammography system. It utilizes electronic detectors to capture X-ray images of the breast, which are then converted into digital format for analysis. FFDM provides high-resolution images with excellent clarity, allowing for detailed examination of breast tissue. Radiologists can manipulate, enhance, and zoom in on specific areas of interest to identify potential abnormalities or early signs of breast cancer. FFDM offers improved detection rates compared to traditional film mammography and is the standard digital mammography modality used in most healthcare facilities.
2. Digital Breast Tomosynthesis (DBT): DBT, also known as 3D mammography, is an advanced form of digital mammography that captures multiple images of the breast from different angles. These images are then reconstructed into a three-dimensional view, providing a more detailed and layered visualization of breast tissue. DBT has shown promising results in improving cancer detection rates and reducing false-positive findings. It is particularly beneficial for women with dense breast tissue, as it helps to reduce the masking effect caused by overlapping structures. DBT has become increasingly popular and is now available in many healthcare facilities as an enhanced digital mammography option.
Both FFDM and DBT have their advantages and limitations. FFDM has been extensively studied and widely adopted, offering excellent image quality and efficient workflow. DBT, on the other hand, provides a more comprehensive view of the breast, reducing the chances of missed abnormalities. However, DBT requires a slightly longer acquisition time and involves higher radiation dose than FFDM. The choice between the two types of digital mammography systems depends on various factors, including the patient’s breast density, the facility’s resources, and the radiologist’s preference.
As technology continues to advance, there may be further developments in digital mammography systems, such as improved image reconstruction algorithms, faster acquisition times, and reduced radiation exposure. These advancements aim to enhance the accuracy and effectiveness of breast cancer screening while prioritizing patient safety and comfort.
What to Expect During a Digital Mammogram
When scheduling a digital mammogram, it’s natural to wonder what to expect during the procedure. Understanding the process can help alleviate any concerns or anxieties you may have. Here’s a step-by-step guide to what you can expect during a digital mammogram:
1. Check-In: Upon arrival at the imaging facility, you will check in at the reception desk. You may be asked to complete some paperwork, provide your medical history, and answer specific questions related to your breast health.
2. Preparation: You will be escorted to a private dressing room and given a gown to wear. It is recommended to avoid using deodorants, powders, or lotions on your underarms or breasts on the day of the mammogram, as these substances can interfere with the imaging process.
3. Positioning: A certified radiologic technologist, specialized in mammography, will guide you to the mammography room. You will be positioned in front of the mammography machine, which typically consists of two plates. The technologist will assist in the proper placement of your breast on the machine’s lower plate.
4. Compression: Breast compression is an essential part of the mammogram. The technologist will gently position and compress your breast between the machine’s plates to spread out the breast tissue. Compression must be firm, but it only lasts for a few seconds during each X-ray image acquisition.
5. Image Acquisition: The technologist will step behind a protective barrier to operate the mammography machine, which will capture the X-ray images of your breast. You will be asked to stand still, hold your breath, and maintain the position for a few seconds while the X-ray is taken. Multiple images may be taken from different angles to capture different views of each breast.
6. Repeat Process for Other Breast: Once the images of the first breast are captured, the technologist will adjust the positioning for the other breast and repeat the compression and image acquisition process.
7. Final Review: After the images are acquired, the technologist will review them to ensure they are clear and adequate for evaluation by the radiologist. If any additional images are needed, the technologist will obtain them at this time.
8. Waiting for Results: You will typically receive your results within a few days. The images will be reviewed by a radiologist who will interpret the mammogram and provide a report to your healthcare provider. If any concerning findings are noted, further diagnostic tests or interventions may be recommended.
During the digital mammogram, you may experience mild discomfort due to the compression of the breast, but it should only last for a few seconds. It’s essential to communicate any concerns or pain to the technologist, as they can adjust the compression as needed to ensure your comfort.
Remember, a digital mammogram is a routine procedure conducted by trained professionals. It plays a crucial role in breast cancer screening and early detection. By knowing what to expect, you can approach your mammogram appointment with confidence and prioritize your breast health.
Is Digital Mammography Better Than Traditional Mammography?
When it comes to breast cancer screening, the question of whether digital mammography is better than traditional mammography often arises. Both methods have their advantages and limitations, and the answer may vary based on individual circumstances. Here’s a closer look at the comparison between digital mammography and traditional mammography:
1. Image Quality: Digital mammography offers superior image quality compared to traditional mammography. The digital format provides high-resolution images with better clarity and detail, enhancing the radiologist’s ability to detect subtle abnormalities or signs of breast cancer.
2. Detection Rates: Numerous studies have shown that digital mammography improves the detection rates of breast cancer compared to traditional mammography, particularly in women with dense breast tissue. The enhanced image quality and advanced image processing techniques of digital mammography make it more effective in detecting early-stage breast cancers and reducing false-negative results.
3. Workflow Efficiency: Digital mammography offers improved workflow efficiency in several ways. The digital images can be instantly viewed and analyzed, eliminating the need for film development and reducing patient wait times. Additionally, digital images can be easily stored, transferred, and accessed for later comparisons, facilitating seamless communication between healthcare providers.
4. Radiation Exposure: Digital mammography typically requires a lower radiation dose than traditional mammography while still delivering high-quality images. This is beneficial for women who require frequent mammograms or those with a higher risk for breast cancer, as it reduces their cumulative radiation exposure over time.
5. Advanced Imaging Options: Digital mammography opens the door to advanced imaging options such as Digital Breast Tomosynthesis (DBT), also known as 3D mammography. DBT provides a more detailed view of breast tissue, reducing the chances of false-positive results and improving the accuracy of cancer detection, especially in women with dense breasts.
6. Availability and Cost: Digital mammography systems have become increasingly available and are now widely used in many healthcare facilities. However, the transition from traditional mammography to digital mammography can come with higher initial costs, including the purchase of digital equipment and software upgrades.
While digital mammography offers several advantages over traditional mammography, it is important to note that traditional mammography is still effective and widely used. In some cases, traditional mammography may be preferred due to cost considerations or the unavailability of digital mammography systems in certain settings.
Risks and Limitations of Digital Mammography
While digital mammography is a valuable tool in breast cancer screening and diagnosis, it is essential to be aware of its potential risks and limitations. Understanding these aspects helps to provide a well-rounded view of the procedure. Here are some of the risks and limitations of digital mammography:
1. Radiation Exposure: Like traditional mammography, digital mammography involves a small amount of radiation exposure. While the radiation dose is typically low and considered safe, repeated exposure over time may have cumulative effects. However, the benefit of early detection and improved outcomes generally outweighs the minimal risks associated with radiation exposure.
2. False-Positive Results: Digital mammography may sometimes lead to false-positive results, meaning that abnormalities are detected on the mammogram that are ultimately found to be non-cancerous. False-positive results can cause unnecessary anxiety and may lead to further diagnostic testing or biopsies, which can be invasive and carry their own risks.
3. False-Negative Results: While digital mammography is highly accurate in detecting breast cancer, there is still a possibility of false-negative results. This means that breast cancer may be present but not detected on the mammogram. Factors like breast density, tumor location, or image interpretation may contribute to false-negative results, emphasizing the importance of regular screenings and follow-up evaluations.
4. Limited Effectiveness in Dense Breast Tissue: Digital mammography may be less effective in women with dense breast tissue. Dense breasts contain more glandular and fibrous tissue, making it more challenging to visualize potential abnormalities on the mammogram. In such cases, additional imaging modalities like ultrasound or magnetic resonance imaging (MRI) may be recommended to improve detection rates.
5. Individual Variations: The accuracy of digital mammography can vary depending on several individual factors, including breast size, breast density, and the ability to hold still during the procedure. These variations underline the importance of personalized care and the expertise of the imaging technologists and radiologists performing and interpreting the mammogram.
6. Cost and Availability: While digital mammography has become more widely available, there are still healthcare facilities that might use traditional mammography due to cost limitations. The transition from traditional to digital mammography may come with initial expenses, including installation, equipment upgrades, and training.
It is vital for individuals to discuss their specific risk factors, concerns, and limitations with their healthcare providers to ensure that they are receiving the most appropriate breast cancer screening and diagnostic tests.
Screening vs. Diagnostic Digital Mammograms
When it comes to digital mammography, there are two main types of exams: screening mammograms and diagnostic mammograms. While both serve a purpose in breast cancer detection and diagnosis, they differ in their objectives, implementation, and target populations. Here’s a closer look at the distinctions between screening and diagnostic digital mammograms:
Screening Mammograms: Screening mammograms are routine exams performed on asymptomatic women who have no signs or symptoms of breast cancer. The primary goal of screening mammography is early detection, capturing breast abnormalities before they become symptomatic. These exams are typically scheduled at regular intervals, based on age and individual risk factors. The aim is to identify breast cancer at an early stage when it is most treatable. Screening mammograms involve taking two X-ray images of each breast, generally from different angles, for comprehensive breast evaluation.
Diagnostic Mammograms: Diagnostic mammograms are performed when there is a known abnormality or an area of concern identified during a screening mammogram or a clinical breast examination. These exams are more detailed and focused, aiming to further evaluate and diagnose specific breast abnormalities. Diagnostic mammograms often involve additional views, such as magnified or spot-compression views, to provide a more comprehensive assessment. The radiologist may also compare the current mammogram with previous ones for comparative analysis.
Digital mammography is an integral part of both screening and diagnostic examinations. However, there are differences in how they are approached and how the images are interpreted. Screening mammograms typically involve a more standardized interpretation process using established criteria and thresholds for detection. Diagnostic mammograms, on the other hand, require individualized assessment and closer scrutiny of specific areas of concern to determine the nature of the abnormality.
It’s important to note that if an abnormality is detected during a screening mammogram, it may necessitate additional diagnostic tests, such as ultrasound or magnetic resonance imaging (MRI), to further evaluate the potential abnormality and guide any necessary interventions. Diagnostic mammograms, on the other hand, may lead to additional imaging and interventions, such as biopsies or aspirations, to establish a definitive diagnosis or rule out any concerns.
Both screening and diagnostic mammograms play essential roles in breast cancer detection and diagnosis. Screening mammograms aim to identify breast cancer early, while diagnostic mammograms provide a more detailed evaluation of known abnormalities. Regular screening mammograms, combined with appropriate follow-up diagnostic procedures, can significantly contribute to early detection and improved outcomes in breast cancer care.
How Often Should You Get a Digital Mammogram?
The recommended frequency for getting a digital mammogram can vary depending on a woman’s age, individual risk factors, and specific guidelines issued by different health organizations. Here are some general guidelines regarding how often you should get a digital mammogram:
1. Age 40 – 49: For women aged 40 to 49, the guidelines differ among various organizations. Some recommend annual mammograms, while others suggest initiating mammography discussions with healthcare providers to assess individual risk factors and make an informed decision based on those factors. It is crucial to consult with your healthcare provider to determine the most appropriate screening plan for you.
2. Age 50 – 74: For women aged 50 to 74, regular screening mammograms every two years are generally recommended by most health organizations. These screenings allow for the detection of breast cancer at an early stage when treatment outcomes are generally more favorable. However, it’s important to note that individual circumstances may warrant a different screening frequency, so consulting with your healthcare provider is crucial.
3. Age 75 and older: The guidelines for women aged 75 and older can vary. Some health organizations suggest continuing with regular mammograms as long as the woman is in good health and expected to live 10 more years or longer. Other organizations acknowledge that the decision to continue screening in older age should be individualized, considering the woman’s overall health, life expectancy, and personal preferences. It’s important to have an open dialogue with your healthcare provider to determine the best course of action.
4. High-Risk Women: High-risk women, including those with a family history of breast cancer or certain genetic mutations like BRCA1 or BRCA2, may require more frequent and earlier mammogram screenings. Such women might benefit from starting regular mammograms at an earlier age, often beginning around 10 years earlier than the age at which the youngest family member was diagnosed with breast cancer. Consultation with a healthcare provider or a specialist can provide personalized guidance based on individual risk factors.
It’s important to understand that these guidelines are general recommendations, and individual circumstances may warrant a different screening approach. Factors such as family history, personal health history, breast density, and specific risk factors should be considered when determining the appropriate screening frequency.
Remember, early detection is key in breast cancer care, so maintaining regular screenings is crucial for identifying any potential abnormalities early on. Open communication with your healthcare provider and adherence to recommended screening guidelines are essential steps towards maintaining breast health.
Digital Mammography for Breast Cancer Screening
Digital mammography is an essential tool in breast cancer screening, detecting potential abnormalities early on and improving outcomes for patients. Here’s how digital mammography plays a crucial role in breast cancer screening:
1. Early Detection: Digital mammography allows for the early detection of breast cancer, often before physical symptoms are noticeable. The high-resolution digital images enable radiologists to identify small calcifications, masses, or other signs of breast cancer that may be present in the breast tissue. Early detection increases the chances of successful treatment and better prognosis.
2. Improved Visualization: Digital mammography provides exceptional image quality and clarity, enhancing the visualization of breast tissue. This allows radiologists to detect subtle changes in breast tissue that may indicate abnormalities or early signs of cancer. The detailed images provided by digital mammography improve diagnostic accuracy and reduce the chances of false-negative or false-positive results.
3. Enhanced Image Manipulation: The digital format of mammograms allows for easy manipulation and enhancement of images. Radiologists can adjust brightness, contrast, and zoom in on specific areas of concern, facilitating a more detailed analysis of breast tissue. This flexibility aids in early detection by revealing subtle abnormalities that may otherwise go unnoticed on traditional mammograms.
4. Streamlined Processes: Digital mammography streamlines the screening process, providing quicker image acquisition and interpretation compared to traditional film mammography. Images can be viewed instantly on a computer screen, eliminating the need for film development and reducing patient wait times. The digital format also allows for seamless storage, retrieval, and sharing of mammogram images, improving communication within the healthcare team.
5. Enhanced Breast Density Assessment: Digital mammography offers improved breast density assessment, which is essential for understanding breast cancer risk. Dense breast tissue can mask abnormalities on mammograms, making them harder to detect. Digital mammography can help radiologists identify breast density accurately, ensuring appropriate screening and potentially leading to supplemental imaging tests in women with dense breasts.
6. Feasibility of Additional Imaging: Digital mammography serves as a foundation for further imaging modalities, such as Digital Breast Tomosynthesis (DBT) or breast ultrasounds. When a suspicious finding is identified on a digital mammogram, additional imaging tests can be performed to provide a more comprehensive evaluation of the breast tissue. These tests aid in confirming or ruling out the presence of breast cancer.
Overall, digital mammography has revolutionized breast cancer screening by improving image quality, enhancing detection rates, and facilitating early diagnosis. Regular digital mammograms, in conjunction with clinical breast exams and self-awareness, provide a comprehensive approach to breast health and early detection of breast cancer.
Digital Mammography for Breast Cancer Diagnosis
Digital mammography plays a crucial role in the diagnosis of breast cancer, providing detailed images that aid in the accurate assessment of breast abnormalities. Here’s how digital mammography is utilized in breast cancer diagnosis:
1. Evaluation of Breast Abnormalities: When a breast abnormality is detected through routine screening or during a clinical examination, digital mammography is often the next step in the diagnostic process. The high-resolution digital images allow radiologists to thoroughly evaluate the abnormality and assess its characteristics. The mammogram helps determine the presence and extent of any lesions or calcifications that may suggest breast cancer.
2. Comparison to Prior Mammograms: Digital mammography is especially useful when comparing current mammograms to previous ones. By reviewing a patient’s history of mammograms, radiologists can identify any changes or developments over time. Analyzing digital images side by side aids in distinguishing between benign changes and potentially cancerous findings, providing valuable information for an accurate diagnosis.
3. Guiding Biopsy Procedures: Digital mammography often plays a crucial role in guiding breast biopsy procedures. When a suspicious breast abnormality is identified, radiologists can use the mammogram images to precisely target the area of concern for biopsy. This helps ensure that the biopsy samples are accurately obtained from the suspicious area, increasing diagnostic accuracy and reducing the need for additional procedures.
4. Monitoring Treatment Response: Digital mammography is used in monitoring patients’ response to breast cancer treatment. Follow-up digital mammograms track changes in the breast tissue to assess the treatment’s effectiveness and identify any signs of recurrence or new abnormalities. Regular digital mammograms provide crucial information to ensure timely adjustments to treatment plans, if necessary.
5. Multimodal Imaging Integration: Digital mammography can be integrated with other imaging modalities in complex cases. Additional imaging tests, such as ultrasound, magnetic resonance imaging (MRI), or molecular breast imaging (MBI), may be performed alongside digital mammograms to obtain a more comprehensive evaluation of the breast. Integrating multiple imaging techniques helps in refining diagnosis and treatment planning.
6. Second Opinion Consultations: Digital mammography makes it easier to share and transmit images among healthcare professionals, facilitating second opinion consultations. Digital mammograms can be easily stored, retrieved, and securely shared electronically, allowing radiologists and oncologists to collaborate and provide expert opinions on complex cases. These consultations ensure thorough evaluation and contribute to accurate diagnoses.
In breast cancer diagnosis, digital mammography provides detailed images that aid in the identification and characterization of breast abnormalities. The ability to analyze and manipulate digital images enhances precision and diagnostic confidence, leading to effective treatment planning and improved patient outcomes.
What Happens After a Digital Mammogram?
After a digital mammogram, several steps are taken to ensure that the results are properly reviewed and appropriate follow-up actions are taken. Here’s a breakdown of what happens after a digital mammogram:
1. Image Interpretation: After the mammogram is performed, a trained radiologist reviews and interprets the digital images. The radiologist examines the images for any signs of abnormality or potential breast cancer. They assess the size, shape, density, and appearance of breast tissue, as well as the presence of any masses, calcifications, or architectural distortions.
2. Preliminary Report and Consultation: Once the radiologist completes the image interpretation, a preliminary report is generated. The report may indicate normal findings, benign changes, or recommend further evaluation. Depending on the facility’s protocol, this preliminary report is often discussed with the patient immediately after the mammogram or provided to the patient’s healthcare provider for further communication and consultation.
3. Additional Imaging: If the radiologist observes an abnormality that requires further assessment, additional imaging tests may be recommended. These tests can include diagnostic mammography with additional views or magnification, ultrasound, or magnetic resonance imaging (MRI). The purpose of these additional tests is to gather more information about the suspicious area and aid in making an accurate diagnosis.
4. Biopsy or Fine-Needle Aspiration: In cases where an abnormality is highly suspicious for breast cancer, a biopsy or fine-needle aspiration may be recommended. These procedures involve obtaining a small tissue sample from the suspicious area to be examined under a microscope. Biopsies and aspirations are typically guided by imaging techniques such as ultrasound or stereotactic mammography, ensuring precise targeting of the abnormal area.
5. Final Report: Once all necessary evaluations, additional imaging, or biopsies are completed, a final report is issued by the radiologist. The report provides a comprehensive assessment of the mammogram findings and any subsequent investigations. The final report is shared with the patient’s healthcare provider to discuss the results and determine the best course of action.
6. Follow-Up Recommendations: Depending on the findings of the mammogram and subsequent evaluations, follow-up recommendations are made. This can include regular surveillance mammograms, further imaging tests at a specified interval, or referral to a specialist for additional evaluation or treatment. Patients are advised to adhere to the recommended follow-up schedule to ensure ongoing monitoring of their breast health.
7. Support and Counseling: Throughout the process, healthcare providers and breast care teams are available to provide support, answer questions, and offer counseling. They understand the emotional impact that breast cancer screening and evaluation can have and are there to provide guidance, reassurance, and thorough explanations of the findings.
It’s important to note that the timeframe for receiving results can vary depending on the healthcare facility and specific circumstances. Patients are encouraged to discuss result timelines and any concerns with the healthcare provider or the radiology department where the mammogram was performed.
Understanding Mammogram Results
Understanding mammogram results is essential to comprehend the findings and implications of the screening or diagnostic test. Here’s a guide to help you understand the different types of mammogram results:
1. Normal/ Negative: A normal or negative mammogram result indicates that no signs of breast abnormalities or cancer were detected. This outcome is reassuring and suggests that no further action or immediate follow-up is required. However, it’s important to note that a negative result does not guarantee the absence of breast cancer, as mammography is not foolproof. Regular screenings are still necessary to ensure ongoing breast health.
2. Benign/ Non-cancerous Findings: Sometimes, mammogram results may show benign or non-cancerous findings. This includes cysts, calcifications, or fibroadenomas, which are common and typically harmless. Benign findings may require ongoing monitoring or additional diagnostic steps, depending on the characteristics of the findings and recommendations from the radiologist or healthcare provider.
3. Suspicious/ Abnormal: If the mammogram reveals an abnormality or suspicious finding, it suggests the presence of a potential breast abnormality that requires further evaluation. This may indicate the need for additional imaging tests, such as diagnostic mammography, ultrasound, or magnetic resonance imaging (MRI), to provide a more detailed assessment of the concerning area. Further investigation is necessary to determine if the abnormality is benign or indicative of breast cancer.
4. Inconclusive/ Indeterminate: In some cases, mammogram results may be inconclusive or indeterminate. This means that the images do not provide a definitive diagnosis and further tests or evaluations are necessary. An inconclusive result may lead to additional imaging or a recommendation for a biopsy to obtain a tissue sample for further analysis.
5. Previous Mammogram Comparison: Mammogram reports often include a comparison to prior mammograms, highlighting any changes or stability in breast tissue over time. This comparison helps radiologists track changes and determine if any new findings have emerged since the last examination.
6. Communication with Healthcare Provider: It’s important to review your mammogram results with your healthcare provider. They can help you understand the findings, answer any questions, and provide guidance on next steps. Your healthcare provider will help interpret the results in the context of your overall health history and guide you through any necessary follow-up procedures or further investigations.
Remember, understanding mammogram results requires careful consideration of the findings in consultation with your healthcare provider. Interpreting the results accurately and taking appropriate actions based on those results are crucial for ongoing breast health and early detection of breast cancer, if present.
Tips for Making Your Digital Mammogram Experience Comfortable
Undergoing a digital mammogram is an important step in prioritizing your breast health. To help make your experience as comfortable as possible, consider the following tips:
1. Choose the Right Facility: Research and select a reputable healthcare facility that specializes in digital mammography. Look for facilities that prioritize patient comfort and have experienced and compassionate staff members who can guide you through the process.
2. Schedule Strategically: Schedule your digital mammogram when your breasts are least sensitive. Avoid scheduling the exam during your menstrual cycle when breasts may be more tender or swollen. This can help minimize discomfort during the compression process.
3. Wear Comfortable Clothing: Opt for a two-piece outfit that is easy to remove and put back on. This allows for convenience during the mammogram procedure and ensures your comfort throughout the appointment.
4. Communicate Any Concerns: Share any concerns or questions you may have with the technologist or radiologist. They are there to address your needs, ensure your comfort, and provide thorough explanations during the mammogram process.
5. Prioritize Relaxation Techniques: Practice relaxation techniques, such as deep breathing or visualization exercises, before and during the mammogram. These techniques can help you relax, reduce anxiety, and make the experience more comfortable.
6. Communicate Your Sensitivity: If you have sensitive breasts or experienced discomfort during previous mammograms, inform the technologist. They can adjust the compression level to a more tolerable level without compromising the accuracy of the results.
7. Distract Yourself: During the mammogram, distract yourself by engaging in activities that take your mind off the procedure. This can include listening to music, reading a book or magazine, or visualizing a calming scene.
8. Be Mindful of Pain Medication: If you anticipate discomfort during the mammogram, consult with your healthcare provider to see if a mild over-the-counter pain reliever is appropriate prior to the procedure. Follow the recommended dosage and timing guidelines provided by your healthcare provider.
9. Seek Support: Consider bringing a support person with you to the appointment. Having someone by your side can provide emotional support and reassurance throughout the process.
10. Take Care of Yourself: After the mammogram, practice self-care. Treat yourself to a comforting activity or reward, such as enjoying a favorite treat or engaging in a relaxing activity that helps you unwind.
Remember, your comfort and well-being are important during a digital mammogram. These tips can help ensure a more comfortable experience, allowing you to prioritize your breast health with ease and peace of mind.